Doctors are increasingly recommending exercise and yoga for osteoporosis patients to reduce their risk of injury and help manage the disease. Exercise improves bone density, relieves discomfort, and reduces the severe impact of this condition.
There are several types of osteoporosis exercises that are useful for managing this disease. Yoga improves posture and balance, thereby reducing the risk of falling. Other exercises also prevent further bone loss, which is crucial for those with decreased bone density.
Patients with osteoporosis should use safe, enjoyable, and effective activities. Before you start any exercise program, consult your doctor or physical therapist.
What is Osteoporosis?
Osteoporosis is a bone disease that develops when bone mineral density and bone mass decrease. It occurs if the structure or strength of the bone changes. Decreased bone strength may increase the risk of broken bones (fractures).
Most people are unaware they have osteoporosis before diagnosis; this silent disease lacks any symptoms. Osteoporosis affects all ages, races, and ethnic groups.
For women, the disease commonly develops a year or two before menopause onset. Certain medications, such as cancer medications, also put people at greater risk.
How to Diagnose Osteoporosis
Osteoporosis is typically diagnosed in a routine screening with your doctor. Health experts recommend regular screening for osteoporosis for women 65 years or older. Women of any age at high risk should receive regular screening.
Men are frequently diagnosed after suffering a fracture. There are currently no guidelines for screening men for osteoporosis.
To increase the chances of an earlier osteoporosis diagnosis, report to your doctor:
- Prior fractures
- Lifestyle (diet, exercise level, alcohol consumption, smoking history)
- Medical conditions that increase fracture risks decrease bone mass
- Family history of osteoporosis or diseases
- Menstrual history (women)
Your doctor may perform a bone mineral density (BMD) test to diagnose osteoporosis. A low BMD results in a diagnosis of osteoporosis. A BMD test can also monitor the effectiveness of ongoing osteoporosis treatment. A treatment plan may include strength or resistance training and yoga for osteoporosis.
After diagnosis, a doctor may recommend lifestyle changes. Exercise, diet, medications, and habit changes work in tandem to promote bone health to reduce your fracture risk.
Osteoporosis Case Studies
Types of Exercises for Osteoporosis
Consider adding exercise to your routine if you have osteoporosis. The following is a list of simple osteoporosis exercises that improve your bone strength, posture, and balance.
Osteoporosis Exercises to Improve Posture
Improved posture benefits those with osteoporosis: it relieves muscular tension and helps manage aches and pains. Poor postural habits increase the risk of spinal compression fractures and need to be corrected.
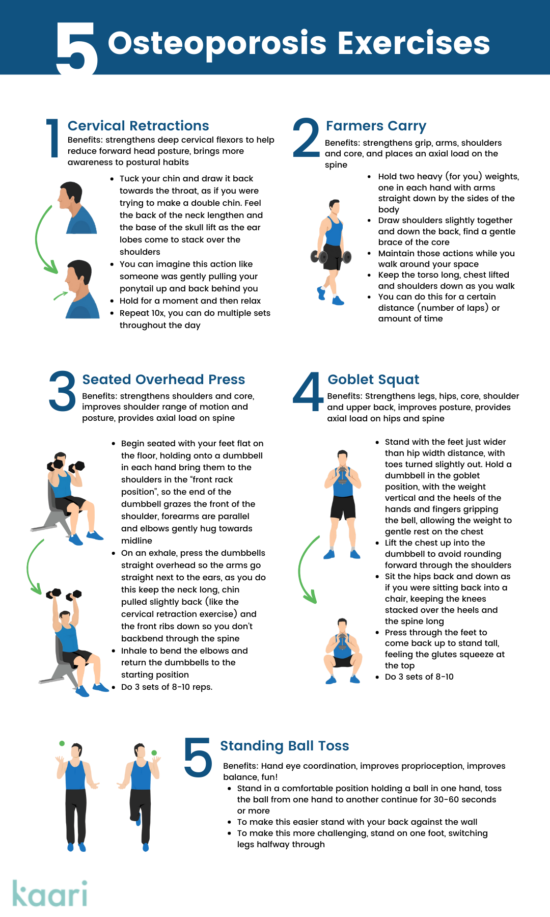
Exercise #1: Cervical Retractions
Benefits: Strengthens the deep cervical flexors, reduces forward head posture, and brings more awareness to postural habits.
- Lightly tuck your chin (like you’re making a slight double chin), and draw it up and back towards the throat. Feel the back of the neck lengthen and the base of the skull lift. The earlobes come to stack over the shoulders.
- Imagine this action like someone is gently pulling your ponytail up and back behind you.
- Hold for a moment, then relax.
- Repeat 10x. Do multiple sets throughout the day.
Axial Loading Exercises for Osteoporosis
Axial loading exercises are designed to load the bones, thereby stimulating them to strengthen in response. This stimulation encourages the bone-producing cells to be more active, thus increasing bone mass and density. Axial loading exercises help you build bone faster.
Exercise #2: Farmers Carry
Benefits: Strengthens grip, arms, shoulders, and core and places an axial load on the spine.
- Hold two heavy (for you) weights, one in each hand, with arms straight down by the sides of the body.
- Draw shoulders slightly together and down the back, and find a gentle brace of the core.
- Maintain actions while walking around your workout area.
- Keep your torso long and chest lifted. Shoulders down as you walk.
- Do this for a certain number of laps or amounts of time.
Exercise #3: Seated Overhead Press
Benefits: Strengthens the shoulders and core and improves shoulder range of motion. It provides an axial load on the spine to increase bone density.
- Begin seated with feet flat on the floor, holding a dumbbell in each hand. Bring them to the shoulders in the “front rack position.” The dumbbell’s end should graze the front of the shoulder, forearms are parallel, and elbows gently hug towards the midline.
- Exhale. Then, press the dumbbells straight overhead, so your arms go straight next to the ears. Keep the neck long and the chin pulled slightly back. Keep the front ribs down to avoid backbend through the spine.
- Inhale while bending your elbows. Return the dumbbells to the starting position.
- Do 3 sets of 8-10 reps.
Exercise #4: Goblet Squat
Benefits: This exercise strengthens legs, hips, core, shoulders, and upper back, improves posture, and provides an axial load on the hips and spine.
- Stand with feet just wider than hip-width distance and toes turned slightly out. Hold a dumbbell in the goblet position, with the weight vertical. The heels of hands and fingers should grip the bell, allowing the weight to rest gently on the chest.
- Lift chest up into the dumbbell to avoid rounding forward through the shoulders
- Sit hips back and down as if you were sitting back in a chair. Keep knees stacked over the heels and the spine long.
- Press through the feet to come back up to stand tall, feeling glutes squeeze at the top
- Do 3 sets of 8-10
Balance Exercises for Osteoporosis
Balance exercises are designed to improve proprioception (your awareness of how your body is positioned in space), reducing the risk of falls.
Exercise #5: Standing Ball Toss
Benefits: Improves hand-eye coordination, proprioception, and balance, and it’s fun!
- Stand in a comfortable position holding a ball in one hand. Toss the ball from one hand to another. Continue for 30-60 seconds or more.
- For an easier version, stand with your back against the wall.
- For more of a challenge, stand on one foot, switching legs halfway through.
Do these exercises every day. Make them a regular part of your fitness routine to help you manage your osteoporosis. These exercises improve your balance, posture, bone density, and strength over time!
8 Yoga Poses for Osteoporosis
Yoga for osteoporosis may be beneficial if done properly and consistently. Yoga improves balance and flexibility and helps reduce the risk of injury, therefore preventing bone fractures.
Here are 8 yoga poses for osteoporosis to try:
Pose #1: Tree Pose (Vrkshasana)
Benefits: Strengthens legs and core while improving balance.
Pose #2: Triangle Pose (Trikonasana)
Benefits: Strengthens legs and back while stimulating abdominal organs.
Pose #3: Side Angle Pose (Utthita Parsvakonasana)
Benefits: Strengthens legs, knees, and ankles while stimulating the abdominal organs.
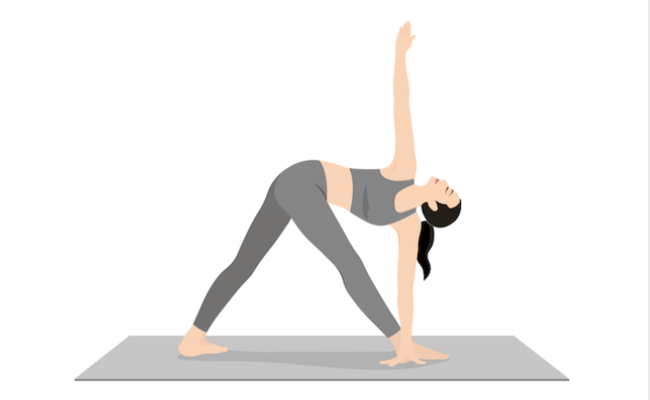
Pose #4: Revolved Triangle Pose (Parivrtta Trikonasana)
Benefits: Improves balance and increases flexibility in shoulders, hamstrings, and upper back, strengthening the legs, ankles, feet, and abdominal muscles.
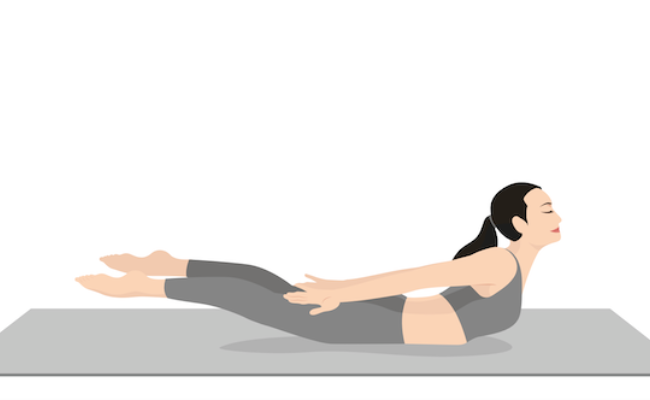
Pose #5: Locust Pose (Salabhasana)
Benefits: Strengthens and increases the flexibility of the back muscles that support the spine. It also increases circulation and strengthens the arms, shoulders, and back.
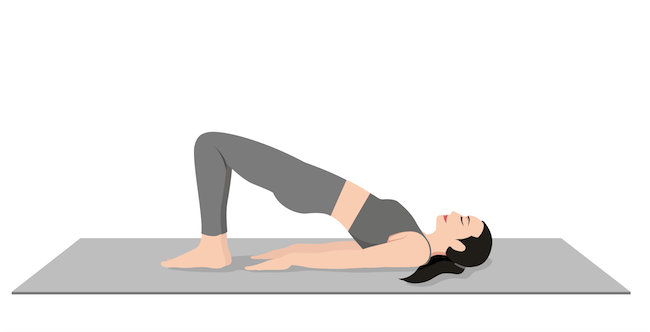
Pose #6: Bridge Pose (Setu Bandha Sarvangasana)
Benefits: Strengthens the back muscles, hamstrings, and glutes. It also improves blood circulation and stimulates the thyroid, lungs, and abdominal organs.
Pose #7: Lord of the Fishes Pose (Matsyendrasana)
Benefits: Strengths the abs and obliques, increases flexibility in the hips and spine.
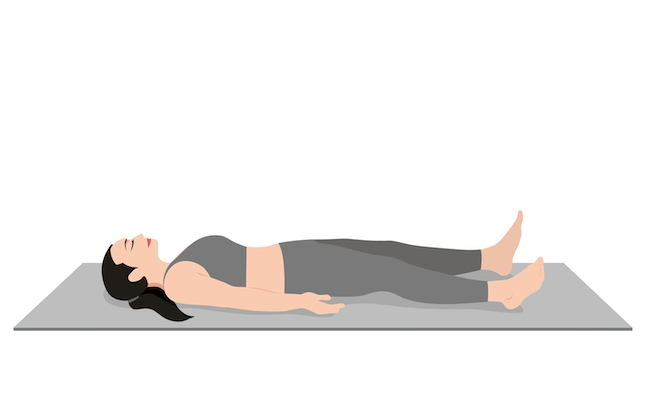
Pose #8: Corpse Pose (Savasana)
Benefits: Reduces stress and fatigue and lowers blood pressure and heart rate.
Which Yoga Poses Are Bad for Osteoporosis?
Before starting yoga for osteoporosis, you should know some poses are contraindicated for people with osteoporosis. Avoid these as they may put you at risk of injury or fracture.
Yoga poses that osteoporosis patients should avoid include:
- Spinal flexion yoga poses cause the back to round. Approach with caution, as they can cause compression fractures.
- Sit-ups and crunches involve spinal flexion and can therefore increase the risk of a compression fracture. Avoid poses that involve bending forward at the waist.
- Handstands place too much body weight on the hands. They increase the risk of a wrist fracture.
- Extreme twists should be avoided by those with osteoporosis. Instead, try a gentle twist in a moderate range of motion to provide helpful stimulation and tension relief for the spine’s muscles.
- Inversions and upside-down poses carry a risk of falling and are not recommended for those with decreased bone density.
- Full backbends and deep backbends place a lot of stress on the spine. However, moderate backbends (e.g. bridge pose and locust pose) strengthen the back.
First, speak with your doctor if you are unsure whether a yoga pose is safe for you. Second, seek guidance from an osteoporosis-informed yoga instructor before doing these poses!
If you are cleared to practice yoga, work with an osteoporosis-informed instructor who can safely modify the poses for your individual needs.
Which is Better for Osteoporosis, Yoga or Pilates?
Is yoga or Pilates better for osteoporosis? Pilates focuses on building core strength and increasing muscle strength. Yoga for osteoporosis focuses on balance and posture.
While both yoga and Pilates are often recommended to osteoporosis patients, health experts found the beneficial effects inconclusive. Neither yoga nor Pilates is proven to be more effective than the other.
However, yoga is associated with a reduced risk of the lower limb and hip fractures in postmenopausal women. Health researchers suggest that Pilates improves BMD.
Starting osteoporosis exercises soon after diagnosis can help you manage the disease.