Long Covid is pandemic’s collateral damage
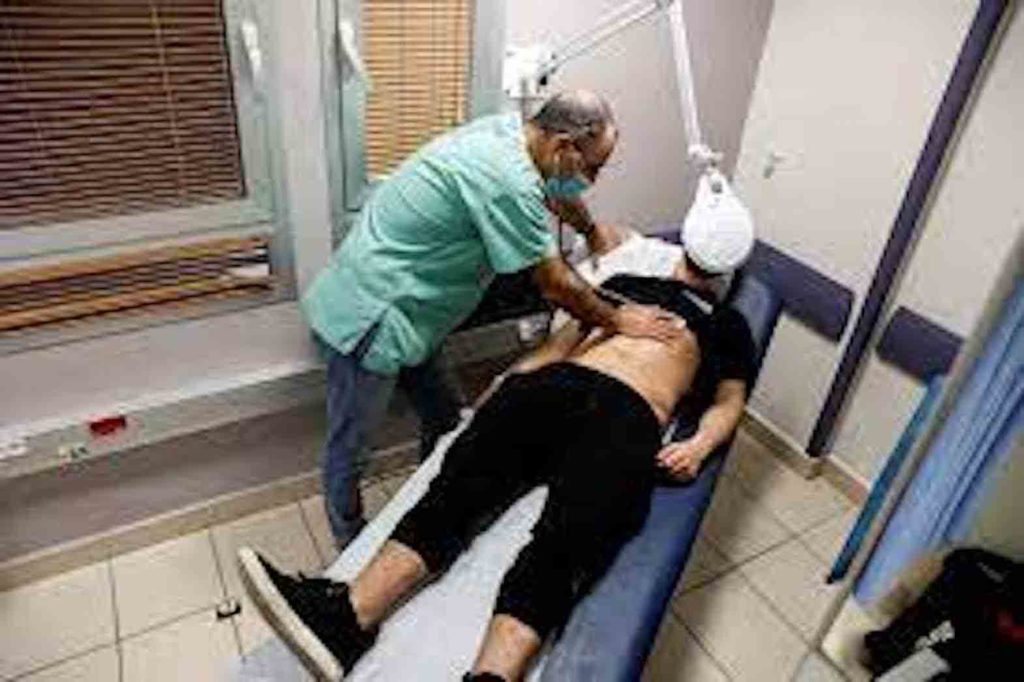
A patient suffering from Long COVID is examined in the post-coronavirus disease (COVID-19) clinic of Ichilov Hospital in Tel Aviv, Israel, February 21, 2022. Picture taken February 21, 2022. REUTERS/Amir Cohen/File Photo
An estimated 4 million people in the U.S. have permanently dropped out of the workforce due to long COVID, which can include an array of symptoms that last well after the initial infection.
Experts say the nation lacks the resources to handle the predicted swell of such cases.
Long COVID is characterized as people experiencing a multitude of symptoms for three months or longer after first being infected. Such symptoms include: tiredness, fatigue, malaise, fever, shortness of breath, brain fog, dizziness, headaches, and sleep disturbance. People also experience psychological symptoms such as depression and anxiety.
More than 21 million Americans have experienced long COVID. A paper released last month in the scientific journal Nature found that almost half of people who had experienced COVID had not fully recovered two months later.
People who have underlying health issues — such as diabetes, hypertension, asthma, and obesity — are at greater risk for developing long COVID. Vaccines and therapeutics taken early in the infection are significant tools in staving off the disease. The three W’s — washing hands, wearing a mask and watching one’s distance from others — are also helpful in preventing infections.
However, lower-income people may lack the ability to access therapeutics in time for it to be effective. Paxlovid, for example, must be started within five days of an infection. And, because of work and living conditions, they may also lack the ability to maintain the distance required to prevent infections.
Few people have availed of the updated booster, also known as the bivalent vaccine. Less than 10% of Californians have taken that shot, according to data from the California Department of Public Health. Nationally, only 20 million people have taken the updated booster, about 8.5% of the total population, according to the Centers for Disease Control and Prevention.
“Four million people not working and not contributing to our economy is a significant burden to our society,” said Dr. Jose Luis Perez, during a news briefing organized by Ethnic Media Services, in partnership with the California Department of Public Health.
Other speakers at the briefing included Dr. Nisha Viswanathan, Director of UCLA’s Long COVID Program; and Michelle Burroughs, Director of Community Engagement and Outreach at the UC Riverside School of Medicine’s Center for Healthy Communities.
Perez is the Chief Medical Officer of the South Central Family Health Center in Los Angeles. His clinic takes in primarily Latino and African American patients that — through their employment — have a high degree of contact with the community, which puts them at higher risk of a COVID-19 infection.
“Symptom control is the bedrock of management,” said Perez, noting that there is no cure for long COVID. The clinic helps its patients access physical therapy, mental health services, and treatments for specific issues brought on by COVID.
“So, no cure. Just let’s make your foggy brain less foggy. Let’s make your joint pain less painful. Let’s try to get you back in some kind of semblance of your normal life. The important thing here is to treat it holistically, treat the person as a whole person,” he said.
Viswanathan, of UCLA’s Long COVID program, agreed with Perez’s approach to managing the illness. Her clinic also employs a symptoms-based strategy to manage fatigue, shortness of breath, brain fog, and the loss of taste and smell, among other issues.
“When we have patients with shortness of breath, for example, we may talk about doing things like pulmonary rehabilitation or breath retraining, which is the idea that you can slowly retrain your diaphragm to take deeper breaths, which can help our patients with that sensation of shortness of breath.”
She added that for many patients struggling with fatigue, “creating a mindfulness practice that incorporates meditation, acupuncture… can be really successful in managing these symptoms.” An anti-inflammatory diet that’s primarily plant based — eschewing meat, sugar, and alcohol, but focusing on whole grains and nuts — can also help with long COVID symptoms.
Both doctors and Burroughs of UC Riverside spoke about the disparities in access to care for long COVID. Perez’s patients may take one or two buses to get to his clinic. Viswanathan’s patients have, on occasion, flown in on private jets. She noted that many low-income patients may not have health insurance that is accepted by the clinic, or may lack the resources to support a healthy diet and mindful practices.
“Black people are not receiving the same quality of care as their white counterparts, and this contributes to a shortened lifespan. Researchers discovered that several severe racial and ethnic disparities have led to higher COVID mortality rates in Black Americans,” said Burroughs.
She also noted that Black people participating in her center’s town halls have reported facing challenges getting their providers to even believe that they have long COVID symptoms. “They feel unheard and they often feel unseen and are sent away not receiving treatment for the symptoms that they presented with,” she said.
“If the Black community continues to not receive proper care, treatment and diagnosis for long haul COVID, it could result in other social injustices like the inability to work, triggering financial instability, which could cause them to lose health insurance and then render them potentially homeless. I know this sounds really extreme, but it’s possible. This has actually happened,” said Burroughs. She noted that providers have often failed to correctly diagnose long COVID for Black people, rendering them unable to qualify for disability insurance.
All three speakers discussed the need to create a pipeline of diverse health care professionals.

